Case studies
Stop Kidney Attack at Sheffield Teaching Hospitals
Share this on – Facebook / Twitter / Linked In


“Stop Kidney Attack!” at STH – Louise Wild RN and Sarah Sampson RN, AKI Nurse Educators and Yvonne Bernes RN, Acute Renal Practitioner at Sheffield Teaching Hospitals describe what they’ve been doing to change practice and raise awareness of AKI.
The Sheffield Teaching Hospitals NHS Foundation Trust is running a Trust wide AKI project. This includes an education programme which aims to better equip Doctors, Nurses and Pharmacists to improve the prevention, identification and management of AKI and associated complications.
How are we implementing this?
- AKI policy
- AKI care bundle checklist and quick reference guide
- AKI Nursing Care Guidelines (NCG)
- ICE alerts from labs highlighting possible AKI (raised creatinine levels from baseline) as per NHS England’s patient safety alert
- Education in high incidence areas first, rolling out across the Trust
The use of the NCG and Care Bundle Checklist assist with the management of AKI and help focus our education with the themes listed below:
- Sheffield Hospitals Early Warning Score (SHEWS); increase frequency to monitor clinical response; patients with high early warning are at greater risk of developing AKI
- Fluids; optimise hydration and improve kidney perfusion
- Urine output;
- Catheter to accurately measure urine output (minimum requirement of 0.5mls/kg/hr)
- Non catheterised patient; has the patient passed urine within 6 or 12 hours and look at ways to assess and measure if this is right for them
- Urinalysis; to detect intrinsic renal disease or infection
- Medications; stop if nephrotoxic, adjust dose if excreted via the kidneys
- Bloods; to monitor kidney function and detect complications such as hyperkalaemia
- Weights; daily to assess for rapid weight gain and hydration
- Documentation; clear record-keeping according to nursing care guidelines and care bundle checklist
We have looked to engage and empower all levels staff to effectively and safely manage their patients. Support and value for the seriousness of AKI helps to facilitate education.
Existing forums to present relevant case based sessions are used. Attending lab alerts facilitates ‘real time’ learning. We try to be as flexible as possible, appreciating the many ways of working and initiatives being rolled out and how AKI prevention, detection and management relate to everyday practice. Issues encountered include staffing and workload pressures. Overall the feedback is good showing enthusiasm for the subject and the need for safer patient care.
The target is to train 25% of Nurses (inpatient areas), Pharmacy and Medical staff within the project time frame (1 year). Personal Achievement and Learning Management System (PALMs) calculate this with staff names recorded when trained. Staff groups are sorted into directorates. Work can be prioritised in areas not meeting targets. Some directorates for nursing show 50% trained while others average around 15%. It is estimated that nearly 80% of pharmacists have had AKI awareness training. The number of medical staff trained has proved more difficult to gauge.
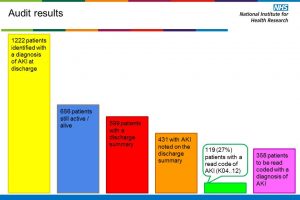
Coding can show the clinical and financial impact of AKI and this should help to show the effectiveness of our project at STH (see Andrea Watson, STH clinical coder’s blog).
Beyond the project time frame we are looking at how to maintain the AKI momentum and continue best practice to optimise patient safety. This is a snapshot some of the ideas we have come up with;
- Champions for each ward area, encouraging them to attend the University of Sheffield (UOS) AKI Study Day. Assist those trained to cascade information and share best practice to other staff
- A quick reference poster provided for each ward to remind everyone of AKI focus points
- Amendments to the SHEWS charts now include AKI, urine output and fluid monitoring prompts
- Development of an eLearning module
- Risk factors alert sticker to be piloted in one acute area to track the patient’s progress
- A two minute desktop animated and text AKI film available to all staff (in collaboration with Andrea Fox at UOS. See also Andrea’s blog)
Case studies